Employee benefits have become a key part of the hiring and retention of employees in today’s hiring market. There is increased stress on compensation as demand for higher salaries and pay rates come from potential hires and the existing workforce.
An employer’s willingness to put the time and effort into their employee’s benefits outside of wages may make the difference. At a high level, total compensation and employee benefits includes, but is not limited to, health insurance, wellness programs, life insurance, and retirement or defined benefit plans.
Health Insurance
Health insurance can provide employees compensation in the form of reducing out of pocket exposure when it comes to their healthcare needs and access to providers.
Health insurance typically accounts for one of the largest Profit & Loss (P&L) expenses for an employer outside of payroll. Typically, there is a cost share for this expense (the insurance premium) between the employees and the employer. Benchmark data from the Kaiser Family Foundation (KFF) stated that in 2025, the average employer share of this expense was 75%, leaving the employees with 25% percent of the premium responsibility deducted out of their payroll. Companies could argue that they are essentially compensating their employees by covering a larger percentage of their health benefits premium on top of what they pay them through payroll.
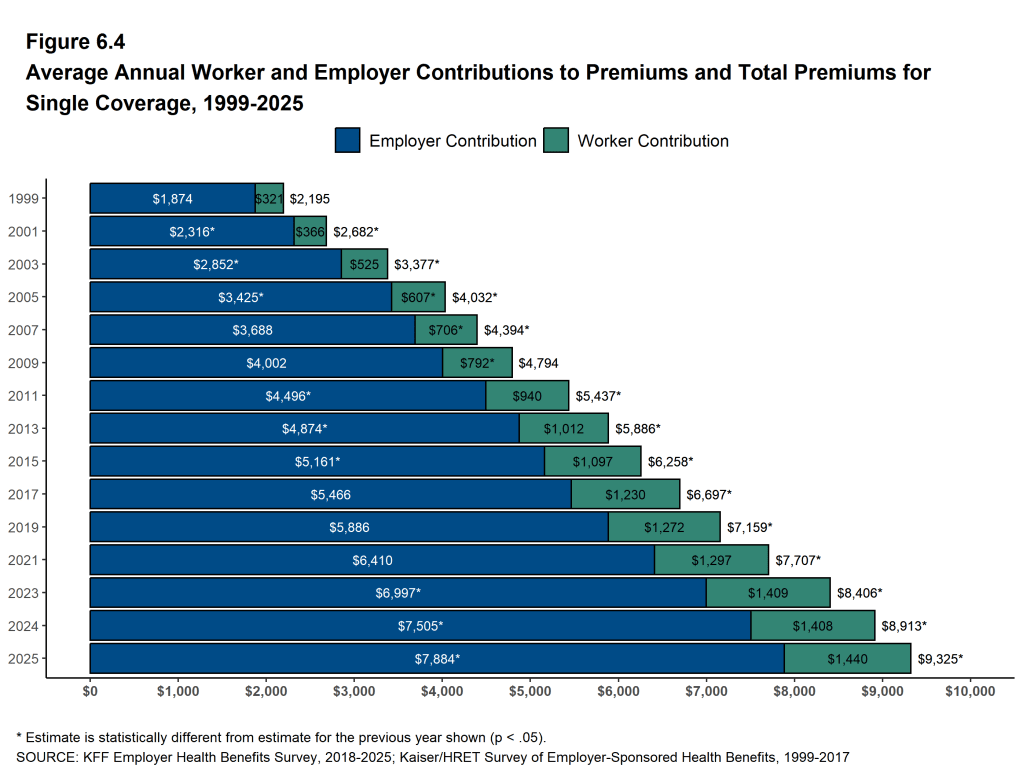
As companies have found it more difficult to create higher payroll, some have decided to take on more of the premium burden, leaving employees with more payroll to spend on other things such as living expenses. However, health insurance premiums have gone up significantly – raising more than seven percent on average.
These renewal increases are driven by a couple primary factors. Among the biggest is the rising cost of prescription drugs overall, the increasing popularity of GLP-1 drugs, and expensive gene and cellular therapies, according to HRExecutive.com.
PPO Vs. HSA Plans – Your Choices May Impact Employee Retention
The receipt of such unfavorable increases has driven companies to reconsider the plans they provide to their employees. Preferred Provider Organizations (PPO) plans offer broader network, copays for doctor’s visits (primary care), as well as specialists covered under the network and prescriptions. Health Savings Account (HSA) plans are high-deductible health plans (HDHP: exceeding $1,400 for individual deductible and $2,800 in family deductible) and require the user to cover the deductible expense out of pocket before the plan contributes to the medical expenses at a coinsurance. PPO plans typically charge higher premiums but require less out of pocket expenses because of their copay structure. HSA plans typically charge less premium but require more of an up-front, out-of-pocket expense to reach the deductible limit. Additionally, they offer the user a pre-tax way to put aside money for qualified medical expenses, defined by the plan.
When faced with such material increases, companies look to transition to plans with cheaper premiums – i.e. higher deductibles, smaller networks (i.e. HMO, EPO, etc.) – and migrate their employees to plans that may create less expense for the company. However, employers often overlook the headache that such a change may cause for their employees. For instance, if you are an employee used to paying a $30 copay for a doctor’s visit under a PPO plan but now must foot the entirety of the doctor’s visit bill until you reach your deductible under an HSA plan, that may cause some stress. Further, if an employer moves to a narrower network to reduce premium, which causes a major local hospital system to be considered out-of-network and not covered by the plan, the HR director will be facing some tough conversations with employees.
These changes, which seem like the right thing to do on the surface, cause more employees to seek other places of employment, even more so than higher wages. Therefore, before making changes in your benefits offerings – carefully analyze your options and potential outcomes. The use of an experienced insurance broker will help do just that.
Many HR professionals have experience with their own population of employees, payroll and benefits at some level. However, the vast differences in health insurance carriers, networks, plans, and benchmarks requires the use of an objective third-party with extensive employee benefits knowledge.
Unison Risk Advisors provides knowledge and skills in the areas of health insurance/employee benefits, commercial P&C insurance, life insurance and retirement plans to our clients. We work with our clients to make informed decisions that can be tough at times – but are backed by data, analysis and market information. We serve thousands of clients nationwide and are among the largest privately held, employee-owned and independent brokerages in the country.
By partnering with Unison Risk Advisors, the company receives the advice they need to make decisions at the leadership level and employees get the assistance they need from a service team to enroll in the right plan for them.